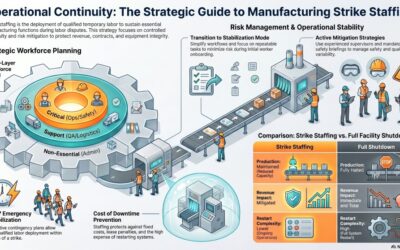
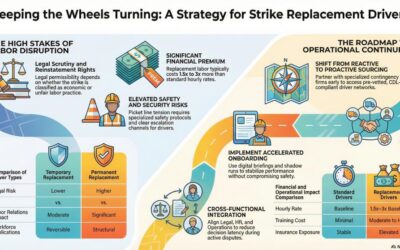
What healthcare workforce contingency planning actually means in operational terms
Healthcare workforce contingency planning is the structured process of maintaining clinical and operational staffing capacity during disruptions without compromising patient safety, regulatory compliance, or care quality.
This planning discipline extends beyond basic staffing backups. It integrates predictive risk modeling, role prioritization, credential validation, and cross-functional coordination to ensure that essential services remain uninterrupted under stress conditions.
Healthcare environments introduce unique complexity due to licensure requirements, scope-of-practice limitations, and patient acuity variability. A contingency plan must therefore define not only who can fill a role, but under what conditions that substitution remains clinically appropriate and legally permissible.
At its core, the objective is continuity of care under constrained staffing conditions. That continuity depends on both pre-identified personnel resources and clearly defined activation protocols that eliminate decision ambiguity during high-pressure scenarios.
Why healthcare systems fail without structured staffing contingencies
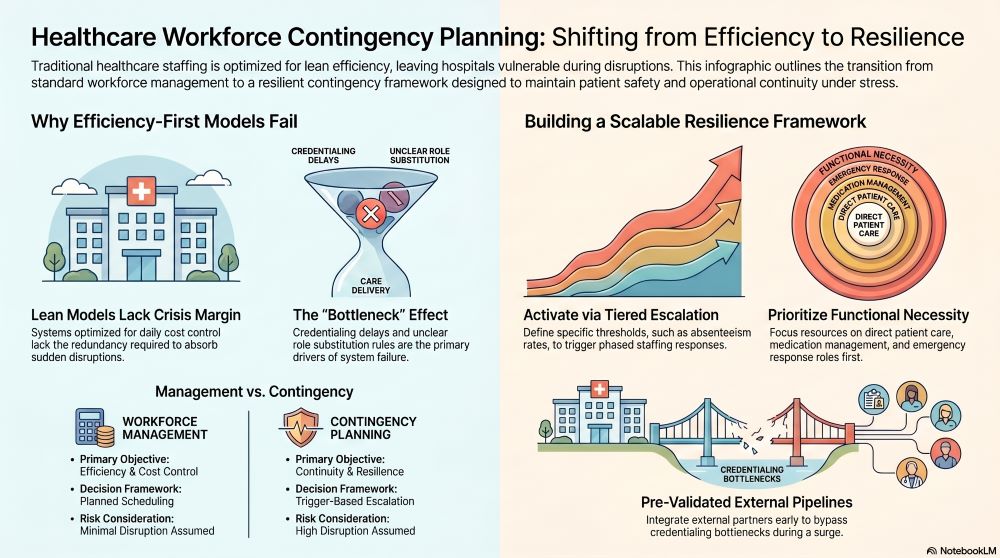
Healthcare systems fail during workforce disruptions because staffing models are typically optimized for efficiency rather than resilience. Lean staffing models leave little margin for variability — when disruptions occur, the absence of predefined escalation pathways leads to reactive decision-making, inconsistent coverage, and increased clinical risk.
Failure points typically emerge in the following areas:
Without formal contingency planning, these failures compound — leading to care delays, increased adverse events, and financial penalties tied to quality metrics.
How contingency planning differs from standard workforce management
Healthcare workforce contingency planning is fundamentally distinct from routine workforce management because it prioritizes disruption response rather than operational optimization. Standard workforce management focuses on scheduling efficiency, cost control, and predictable demand. Contingency planning, by contrast, assumes instability and designs systems that remain functional under abnormal conditions.
| Dimension | Workforce Management | Contingency Planning |
|---|---|---|
| Primary Objective | Efficiency and cost control | Continuity and resilience |
| Time Horizon | Short- to mid-term | Immediate to crisis-driven |
| Staffing Model | Fixed or predictable | Flexible and scalable |
| Decision Framework | Planned scheduling | Trigger-based escalation |
| Risk Consideration | Minimal disruption assumed | High disruption assumed |
| Resource Allocation | Optimized for baseline demand | Reserved for surge capacity |
| Compliance Focus | Standard credentialing cycles | Accelerated and pre-validated pathways |
This distinction explains why organizations that perform well under normal conditions can still struggle during disruptions. Efficiency-focused systems lack the redundancy and flexibility required for crisis response.
Which roles must be prioritized during staffing disruptions
Prioritization is not based solely on job titles. It is determined by the functional necessity of each role within care delivery pathways.
Critical roles in healthcare contingency planning are defined by their direct impact on patient outcomes, regulatory compliance, and operational continuity. Key role categories include:
How to build a scalable healthcare staffing contingency framework
A scalable contingency framework is built by aligning workforce flexibility with predefined activation logic and validated staffing pipelines. The framework must function as a system rather than a document — each component should be operationally executable without reinterpretation during a crisis.
Core framework components
Risk scenario mapping
Identify disruption types — pandemics, labor shortages, natural disasters, and system outages — before they occur.
Trigger-based activation thresholds
Define specific conditions — such as absenteeism rates or patient census spikes — that activate contingency measures.
Tiered staffing escalation model
Structure staffing responses in phases, from internal redistribution to external workforce deployment.
Pre-credentialed staffing pools
Maintain access to licensed professionals who can be deployed without onboarding delays.
Cross-training and role flexibility
Expand internal capacity by training staff for adjacent roles within scope-of-practice limits.
Command and communication structure
Establish a centralized decision authority with clear reporting lines across all teams.
A framework without pre-validated execution paths introduces delays that negate its purpose. Planning must translate directly into action without additional approval layers during activation.
The role of external staffing partners in maintaining continuity
External staffing partners provide surge capacity that internal systems cannot generate quickly enough during workforce disruptions. Healthcare organizations rely on external resources to bridge gaps created by sudden demand spikes or internal workforce shortages — however, the effectiveness of these partnerships depends on pre-established integration rather than ad hoc engagement.
Effective external staffing integration requires:
Organizations that engage external staffing reactively often encounter delays, higher costs, and inconsistent staff quality. Structured partnerships mitigate these risks by ensuring readiness before disruption occurs.
Key risks that undermine contingency workforce plans
Healthcare workforce contingency plans fail when assumptions do not align with real-world constraints. Several risk categories consistently degrade plan effectiveness:
Operational Risks
Compliance Risks
Human Factors
Financial Risks
Mitigation requires continuous plan testing, scenario simulation, and refinement based on observed performance.
How healthcare organizations evaluate contingency readiness
Contingency readiness is measured through the organization’s ability to maintain care standards under simulated or real disruption conditions. Evaluation frameworks typically include both quantitative and qualitative indicators.
Key readiness metrics
Time-to-fill critical roles
Measures how quickly essential positions are staffed during disruption.
Staffing coverage ratio under surge
Evaluates alignment between patient demand and available workforce.
Compliance adherence rate
Tracks whether regulatory requirements are maintained during activation.
Clinical outcome stability
Assesses whether patient outcomes remain consistent under stress conditions.
Staff utilization efficiency
Measures workload distribution across available personnel.
Testing methods
Organizations that rely solely on documentation reviews often overestimate readiness. Practical execution testing reveals operational gaps that static plans cannot identify.
Practical strategies for improving workforce resilience
Workforce resilience in healthcare is achieved through redundancy, flexibility, and sustained workforce engagement. Several strategies consistently improve resilience outcomes:
01
Develop internal float pools
Dedicated staff trained to operate across multiple departments reduce dependency on external resources.
02
Implement predictive staffing analytics
Use historical data to anticipate staffing shortages before they occur.
03
Standardize rapid onboarding processes
Reduce time required to deploy external or reassigned staff through pre-built documentation and credentialing pathways.
04
Strengthen retention and engagement programs
Reduce turnover and maintain institutional knowledge within the organization.
05
Establish regional staffing collaborations
Share workforce resources across healthcare networks to increase surge capacity without added overhead.
06
Invest in telehealth and remote care capabilities
Reduce dependency on physical staffing presence for eligible care functions.
07
Create structured rest and recovery protocols
Maintain workforce performance and prevent burnout during extended disruptions.
FAQ: Healthcare workforce contingency planning
What is the primary goal of healthcare workforce contingency planning?
The primary goal is to maintain safe, compliant, and effective patient care during staffing disruptions.
How is contingency staffing different from overtime scheduling?
Contingency staffing involves structured escalation and external resources, while overtime relies on existing staff capacity.
When should a contingency plan be activated?
Activation should occur when predefined thresholds — such as staffing shortages or patient surges — are reached.
Can non-clinical staff be used in clinical roles during emergencies?
Only within legally permitted scope-of-practice boundaries and with appropriate training.
Why is pre-credentialing external staff important?
It eliminates onboarding delays and ensures immediate deployment capability when a disruption occurs.
How often should contingency plans be updated?
Plans should be reviewed and updated regularly, especially after drills or real-world activation events.
What role does technology play in contingency planning?
Technology enables real-time workforce visibility, predictive analytics, and coordination across teams.